Health-&-Fitness
Self-care Tips for Parents of Newborns
Welcoming a newborn into the family is undoubtedly a joyous occasion, but it also comes with its share of challenges and adjustments. New parents often find themselves having sleepless nights, with endless diaper changes, and the overwhelming responsibility of caring for a tiny, fragile human being. Amid these changes, parents often neglect their equally important well-being. But self-care for parents is essential. Let's take a look into some self-care tips for new mums and dads.
What is Self-Care?
Self-care for parents of newborns involves intentional actions to preserve their physical and emotional well-being amid the challenges of early parenthood. It encompasses activities that promote rest, nutrition, and emotional resilience.
Self-care acts as a protective shield. From prioritising quality sleep to maintaining a balanced diet, self-care is vital for navigating the demanding responsibilities of caring for a newborn.
Read more: 10 Ways to Ensure Emotional Well-being during Pregnancy
Why is it Essential for New Parents to Take Care of Themselves
The physical toll of caring for a newborn is undeniable. Lack of sleep, irregular eating patterns, and constant physical demands can lead to exhaustion and potential health issues. Prioritising self-care ensures parents can maintain the physical stamina needed for the demanding tasks at hand.
Emotional well-being is equally crucial. The rollercoaster of emotions that accompany parenthood, from joy to frustration, can be overwhelming. Taking time for self-care enables parents to recharge emotionally, fostering a healthier mindset to face the challenges with resilience.
Essential Tips for Caring Parents of Newborns
Prioritise Quality Sleep
Ensuring sufficient, quality sleep is crucial for both physical and mental well-being, especially as new parents grapple with inevitable sleep deprivation. To make a significant difference, one should create a sleep schedule that allows for restful nights.
Read more: 15 Gift Ideas for a Newborn Baby
Parents may consider taking turns with their partner during nighttime duties to maximise the quality of their rest. This approach not only fosters a supportive partnership but also ensures both parents have opportunities for uninterrupted and rejuvenating sleep amidst the demands of caring for a newborn.
Delegate Responsibilities
Due to traditional mindsets and patriarchal social systems, in many families, the care of a newborn and doing household chores are granted as the mother's sole responsibility. It may deteriorate the mother’s emotional and physical health. As a result, many mothers suffer postpartum depression. Therefore, it is necessary to recognise that the mother of the baby need not shoulder everything alone; seeks the aid of her partner, family, and friends.
The new parents and other family members can share diverse responsibilities like household chores, cooking, cleaning, etc. Delegating responsibilities eases the burden and also grant parents precious moments to concentrate on both nurturing their newborn and tending to their well-being.
Read more: Newborn Baby, Infant Care Tips during Summer
Building a supportive network ensures that the challenges of early parenthood are shared. It fosters a healthier and more balanced environment for both parents and their new addition to the family.
7 Types of Strength Training And Their Benefits
The American Council of Exercise outlines seven diverse forms of strength training, each catering to distinct functional applications. While each type enhances physical fitness, athletic abilities, or overall well-being, their stark differences explain why a track runner and a bodybuilder, both labeled "strong" and "fit," frequently exhibit contrasting appearances and training routines.
What is Strength Training?
Strength training, also called weight or resistance training, involves doing exercises to get stronger and last longer. It's not just about lifting weights; you can use your body weight or try different exercises like isometrics and plyometrics. The goal is to make your muscles stronger over time.
Strength training is mainly a type of exercise that doesn't require a lot of air, but some forms like circuit training also get your heart pumping. It helps make your muscles, tendons, and bones stronger, boosts metabolism, and reduces the chance of getting hurt. Athletes and older people can benefit from it to improve their joints, hearts, and lower their injury risk. Many sports and activities include strength training in their practice to make people better at what they do.
Read more: How Does Physical Activity and Exercise Affect Testosterone Levels?
Benefits and Risks of Different Types of Strength Training
Agile Strength Training
Agile Strength Training is a fitness approach that blends traditional strength exercises with practical movements for daily activities. It emphasizes adaptability and flexibility, incorporating dynamic workouts like weightlifting, bodyweight exercises, and flexibility drills. The primary goal is to enhance overall strength, flexibility, and agility, adapting to individual needs and progress.
Benefits of Agile Strength Training
This approach improves overall strength, flexibility, and the ability to move with precision in different directions. It's valuable for daily tasks, promoting quick and controlled responses to your surroundings, ultimately aiding injury prevention.
Read more: Why You Should Try Walking Backwards
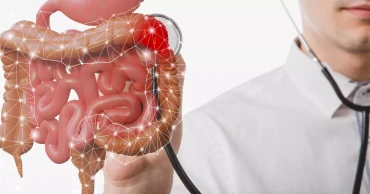
Colon Cancer: Everything You Need to Know
Colorectal cancer, or colon cancer as it is commonly known, is a type of cancer that develops at the rectum or colon of the human body. WHO reports that colon cancer is the third leading type of cancer globally with 10% of all reported cases. It is also the third highest reason for cancer-related deaths. Let’s take a detailed look into the fatal disease, what causes it, and how people can potentially save themselves from colon cancer.
How Does Colon Cancer Develop?
The colon or the rectum is the terminal point of the digestive system. It is essentially a sac that houses the bowel and aids in the bowel movement process. The lining of the colon can develop precancerous polyps which can become cancerous over time.
It is important to note that all polyps are not cancerous. However, it is needed to medically treat them at the earliest as there is always the chance of it developing into cancer cells.
The exact cause of polyp development is unknown. However, scientists have often pointed out that genes and age play a crucial role in their development. Other factors like diets, obesity, smoking, and inflammation of the colon lining have been identified as leading causes thus far.
Read more: Measles: Causes, Symptoms and Prevention
What are the Symptoms and Causes of Colon Cancer?
Symptoms of colon cancer include:
Change in Bowel Movement
As a precursor to colon cancer, a patient often notices a significant shift in bowel movement. For example, the frequency of diarrhea, constipation, or a change in stool consistency is noticed.
Blood Discharge
A common symptom of colon cancer is the presence of blood in the stool. Patients may not feel any apparent discomfort but dark tarry stools may be noticed during bowel movement.
Pain in the Abdomen
Another common symptom of colon cancer is severe and lasting pain in the abdomen. It generally starts as mild discomfort and gradually moves to severe cramps.
Read more: JN.1: Symptoms, Prevention of and Precautions for the New COVID-19 Variant
Anemia
The blood discharge with stool may trigger anemia or loss of red corpuscles in the blood. Anemia also triggers weakness and fatigue which is a secondary symptom of colon cancer.
Unexpected Weight Loss
Another sign of any cancer in general is the unexpected loss of weight. Cancer patients including colon cancer ones tend to rapidly lose weight which may lead to secondary complications.
There are several known causes of colon cancer. These include:
Age
Age is one of the commonly identified factors behind colon cancer. Anyone over the age of 50 is at risk of contracting colon cancer though it might occur at any age.
Read more: Foods that Help Relieve Nausea and Vomiting
Family History
Genetics are also thought to be a reason behind colon cancer. Families with a history of Familial Adenomatous Polyposis or FAP and Lynch Syndrome tend to compound the chances of contracting colon cancer.
Personal Medical History
Colon cancers are often recurring, meaning they can come back even if it is treated completely. A personal medical history of colon cancer or repeated polyp formation may trigger renewed cancer cell generation in the colon linings.
Additionally, Inflammatory Bowel Diseases or IBDs like ulcerative colitis and Crohn’s disease increase the risk of contracting colon cancer. Patients with Type 2 diabetes also run the risk of developing colon cancer.
Read more: 10 Dengue Myths Debunked: Here are the Facts
How Does Physical Activity and Exercise Affect Testosterone Levels?
Testosterone, a crucial hormone for both men and women, plays a vital role in various bodily functions. One factor that significantly influences testosterone levels is exercise and mental well-being. So, it is natural to wonder how these two interact. Let's explore the intricate relationship between exercise and testosterone to understand how physical activity impacts hormonal balance.
What is Testosterone?
Testosterone, a pivotal hormone, is present in both men and women, although commonly associated with male characteristics. Produced in the testicles in men, ovaries in women, and to a lesser extent, the adrenal glands, it plays a crucial role in diverse bodily functions.
This hormone is instrumental in the development of male reproductive tissues, including the testes and prostate. Often referred to as the "male sex hormone," testosterone acts as a conductor orchestrating various bodily functions, impacting muscle growth, bone density, mood, libido, and more.
Read more: 10 Hazards at the Gym and How to Avoid Them
In women, testosterone is essential for maintaining reproductive health and influencing aspects of mood and energy.
The decrease of testosterone hormone with age is natural, but factors like stress and lifestyle can accelerate this process. Understanding how to optimise testosterone, perhaps through targeted physical exercises, can help promote overall health and well-being.
How Exercise Affects Testosterone
Relationship between Exercise and Testosterone
The correlation between exercise and testosterone levels in men has been well-established by different research initiatives. Long-term engagement in physical activity has shown a consistent increase in testosterone levels.
Interestingly, certain physical exercises can induce a temporary spike of testosterone hormone within fifteen minutes to an hour after completion of the workout. Such short term impacts are especially noticeable in younger men. This immediate boost is more pronounced when workouts are performed in the morning, aligning with the natural peak of testosterone levels during that time.
Read more: Zumba: Dance Your Way into Fitness
However, sustaining elevated testosterone levels over the long term requires regular exercise. While there is currently no conclusive evidence of increased testosterone levels in women due to exercise, the presence of testosterone during workouts aids in training and muscle recovery.
Research reveals nuanced findings show that men experience significant testosterone increases post-weightlifting, whereas women show minimal changes. Resistance training in women has a temporary testosterone boost impacting fat distribution.
For older men, regular physical activity not only raises testosterone levels but also enhances growth hormone levels and positively affects brain function. In those previously inactive, exercise led to a notable increase in dihydrotestosterone (DHT).
Read more: 10 Great Health, Fitness Career Ideas You May Consider
Interestingly, even in men with obesity, regular exercise proved more effective in boosting testosterone levels than weight loss diets alone. Maintaining healthy or heightened testosterone levels is crucial, not just for muscle building but for overall well-being and exercise progress.
Exercises that Increase Testosterone
Not all exercises can create the same impacts when it comes to elevating testosterone levels. Understanding the most effective workouts can contribute significantly to achieving the desired hormonal balance. Here is a closer look at some of the best exercises known to increase testosterone.
Measles: Causes, Symptoms and Prevention
Measles, a highly contagious viral infection, has been a persistent health concern worldwide. Understanding the symptoms and causes of measles is crucial for individuals and communities to combat its spread effectively. In the wake of a recent measles outbreak in Europe, understanding the symptoms and causes of this highly contagious viral infection is more crucial than ever.
What is Measles? How Does It Affect People?
Measles is characterised by fever, cough, and a distinctive rash. The virus responsible for measles is a paramyxovirus (known as rubeola), and its high contagiousness often leads to outbreaks, especially in areas with low vaccination rates. This contagious viral disease easily spreads through respiratory droplets when an infected person breathes, coughs, or sneezes.
While capable of affecting anyone, it predominantly targets children. Measles initiates in the respiratory tract and then disseminates throughout the body. As a highly contagious disease, it underscores the importance of preventive measures, with vaccination being the most effective way to shield against severe illness, complications, and potential fatalities.
Read more: Foods that Help Relieve Nausea and Vomiting
What are the Symptoms of Measles?
The symptoms of measles typically manifest 10–14 days after exposure to the virus, with a prominent rash being the most evident sign. Early symptoms persist for 4–7 days and include
- A high fever- Runny nose - Cough - Red and watery eyes - Tiredness- White spots inside the cheeks, known as Koplik's spots
The characteristic rash emerges approximately 7–18 days post-exposure, starting on the face and upper neck, and gradually spreading to the hands and feet over about 3 days. This rash persists for 5–6 days before fading. Other measles symptoms may include
- A sore throat- White spots in your mouth- Muscle pain- Sensitivity to light.
Read more: Which Vitamins are Essential for Women?
What are the Causes of Measles?
The measles virus, belonging to the Paramyxoviridae family, is renowned for its highly contagious nature. Spread primarily through respiratory droplets, it easily transmits from person to person. Measles is exceptionally contagious, with individuals at risk of contracting the virus even after an infected person has left the vicinity.
The virus can endure on surfaces and in the air for hours, posing a continual threat. Originating in the nose and throat, measles is transmitted when an infected person coughs, sneezes, or talks, releasing infectious droplets into the air. These droplets, both airborne and on surfaces, remain contagious for several hours, facilitating the virus's easy transmission.
Measles Health Risks
The primary cause of death resulting from measles is often complications associated with the disease. These complications encompass various serious issues
- Blindness- Encephalitis, an infection leading to brain swelling and potential brain damage- Severe diarrhea, accompanied by dehydration- Ear infections- Severe respiratory problems, including pneumonia.- In the case of a pregnant woman contracting measles, it poses a significant risk, endangering both the mother and potentially resulting in premature birth with a low birth weight for the baby.
Read more: How to Protect Babies and Children from Dengue Fever
Complications, often leading to fatalities, are more prevalent in children under 5 and adults over 30, especially those malnourished or with weakened immune systems, as measles itself can compromise the body's ability to defend against infections, rendering children exceptionally vulnerable.
JN.1: Symptoms, Prevention of and Precautions for the New COVID-19 Variant
The past two years have been a rollercoaster ride of uncertainty, and just when the world thought the situation of Coronavirus pandemic was under control, a new variant, JN.1, has surfaced. This article aims to dissect the symptoms, causes, and implications of JN.1, the new strain of COVID-19.
What is JN.1? How Does it Affect People?
JN.1, an Omicron subvariant, surfaced in September last year amid declining temperatures, showing heightened transmission rates. Stemming from BA.2.86 (also known as Pirola), JN.1 possesses an additional spike protein mutation crucial for SARS-CoV-2 cell interaction.
The World Health Organization (WHO) categorises JN.1 as a Variant of Interest (VOI), distinct from its precursor BA.2.86, due to its rapid spread. Recently identified in the United States, close monitoring is essential to comprehend and address the dynamics of this evolving COVID-19 variant.
The rise in JN.1 cases aligns with a general surge in COVID-19 infections. Symptoms of JN.1 infection closely resemble those of earlier Omicron variants, with no apparent increase in severity. While there are hints of potential increased diarrhoea cases, concrete data supporting this observation is currently lacking. Continuous monitoring is essential to better understand the characteristics of this variant.
Read more: Bangladesh reports 53 more Covid-19 cases in 24hrs
Is JN.1 More Transmissible?
JN.1, a descendant in the Omicron lineage, appears to be more transmissible than its precursor, BA.2.86. The observed surge in case numbers indicates increased transmissibility. Several newer variants, including JN.1, exhibit mutations affecting the spike protein's binding strength to respiratory cells, potentially enhancing replication and immune evasion.
While it remains early to precisely gauge JN.1's transmissibility and immune escape compared to other Omicron variants, experts assert its notable virulence. Dr. Joseph Khabbaza from the Cleveland Clinic notes that the current strain seems to deliver a more potent impact than its predecessors.
Who is at High Risk of Infection?
Certain groups face a higher risk of contracting the easily transmissible virus. These include:
- People aged 65 and above- Diabetic people- People with neurological disorders- People who have pre-existing health conditions like COPD, heart diseases, chronic kidney diseases, cystic fibrosis, and individuals suffering from liver ailments- Pregnant women- Smokers- People with a compromised or weak immune system- Healthcare workers- People who are not vaccinated or have not taken booster shots.
Read more: COVID-19: Bangladesh reports 35 more cases in 24hrs
What are the Symptoms and Causes of the JN.1 COVID-19 Variant?
JN.1's increasing prevalence implies heightened contagiousness or improved evasion of immune defences, as per the CDC. Currently, there is no evidence indicating it induces more severe disease than other strains, despite potential transmission spikes. Symptoms associated with JN.1 seem comparable to those induced by other strains, encompassing a range such as
- Sore throat- Congestion- Runny nose- Cough- Fatigue- Headache- Muscle aches- Fever or chills- Loss of sense of taste or smell- Shortness of breath or difficulty breathing- Nausea or vomiting- Diarrhoea
The nature and intensity of symptoms typically rely more on an individual's overall health and immune condition rather than the specific variant causing the infection.
Read more: COVID-19: Bangladesh reports 28 more cases in 24hrs
How Does Fat Leave the Body When We Lose Weight?
Losing weight is a common goal for many, but have you ever wondered where the fat goes when you shed those kgs? This article will unveil the secrets of fat-burning and discover effective weight-loss strategies. Join the journey to a healthier you, where every lost kg tells a tale of determination and transformation.
What is Body Fat?
Body fat, often unappreciated, serves a crucial role as a reservoir of stored energy, particularly during extended periods without food access. Body fat refers to the adipose tissue present in the human body, serving as a crucial energy reserve and playing various physiological roles.
Comprising triglycerides, body fat is stored in adipocytes, or fat cells, distributed throughout the body. While essential for insulation, organ protection, and hormone regulation, an excess of body fat can lead to health issues.
Read more: 10 Delicious Quinoa Recipes for Weight Loss
The growth of fat cells in size and number is determined soon after birth and during adolescence. It remains relatively stable in adulthood unless disrupted by long-term excess calorie consumption. Weight loss can shrink fat cells but not their number.
Body fat is typically categorised into two types: essential fat and storage fat. Essential fat is vital for normal physiological functioning, found in organs, nerves, and cell membranes. Storage fat, on the other hand, accumulates beneath the skin (subcutaneous fat) and around organs (visceral fat), providing a reserve for energy needs.
Measuring body fat percentage is crucial for assessing overall health and fitness. Various methods, such as skinfold calipers, bioelectrical impedance, and dual-energy X-ray absorptiometry (DEXA), help estimate body fat content. Healthy body fat percentages differ based on age, sex, and fitness levels, with excessive body fat linked to increased risk of conditions like obesity, cardiovascular diseases, and diabetes.
Read more: How to Lose Weight without a Strict Diet or Heavy Exercise
Maintaining a balance between essential and storage fat is essential for overall well-being. It apexes the importance of a healthy lifestyle encompassing proper nutrition, regular exercise, and holistic health management.
Popular Motorcycle Helmets Under 15000 Taka in Bangladesh
As a convenient personal transport, the popularity of motorbikes is on the rise. However, bike riding can pose a threat if not wearing safety gear, especially the helmet. Motorcycle helmets come in all types of shapes and sizes. From half helmets to modular, off-road, dual-face to full-face helmets, the choice seems to be endless. But in addition to the types, there’s also the aspect of QC and compliance to consider. While it might be difficult to fit all the criteria in a budget helmet, here’s a list of the ones to consider under 15000 BDT.
What to Consider Before Buying a Motorbike Helmet
In Bangladesh, The Road Safety Act of 2018 mentions the requirement of a “proper” bike helmet for the rider and the pillion. But there’s no exact specification to define what’s “proper.” As a result, helmets as cheap as 600 BDT are easily available in the market. But none of those qualify for the UN or the ECE standards.
Before getting into the list, here’s what one should consider before buying a motorcycle helmet.
Safety Standards
As mentioned above, there aren’t any strict measures to enforce standards on motorcycle helmets. But considering personal safety, look for helmets that meet either ECE, UN, or BSTI standards or clearance certification.
Read more: 10 Best GPS Trackers for Motorcycles in Bangladesh
Fit and Comfort
There’s a common misconception that helmets need to be tight fit. On the contrary, the best approach is to go for a snug fit that sits comfortably level with the head. Even the pin-lock should be adjusted in a way that it doesn’t obstruct the natural jaw movement.
Helmet Type
The most common types of helmets in Bangladesh are full-face and open-face helmets. There are also modular ones but those are better suited for cruiser or off-road bikes. For normal city commutes, a full-face or open-face helmet would be ideal.
Weight
Always opt for a lightweight helmet so as not to stress out your head or shoulder. As a rule of thumb, look for a combination of lightweight build and enough cushioning for a snug and comfortable fit. Fiberglass or polycarbonate helmets can be a great choice in this regard. There are also carbon fiber ones, but those won’t come under 15000 unfortunately.
Read more: Uber Driver Account in Bangladesh: How to Activate, Delete, and Reactivate
Noise Level
Make sure the helmet has ample aerodynamic and wind noise reduction for a comfortable ride. It depends on the fit and how much noise can be blocked. Too tight a fit might block essential sounds as well which might become an accessory for accidents. So try and strike a balance in between.
Why You Should Try Walking Backwards
Walking, a seemingly straightforward activity, has taken a new twist — a backward or reverse step. The concept of walking backwards, often overlooked, comes with many benefits that can significantly enhance your physical and mental well-being. Let's delve into the world of backward strides and explore why incorporating this unique practice into your routine could be a game-changer.
Health Benefits of Reverse Walking
Physical Benefits
Improves Balance and Gait
Walking backwards challenges your brain and body to coordinate in new ways, which can improve your overall balance and stability. This practice can be especially beneficial for senior citizens or people who are recuperating from injuries.
Reduces Knee Pain and Strengthens Muscles
By engaging different muscle groups than forward walking, walking backwards can take stress off your knee joints and strengthen your hamstrings, calves, and glutes. This can be helpful for people with knee pain, arthritis, or weak lower body muscles.
Read more: How to Lose Weight without a Strict Diet or Heavy Exercise
Increases Flexibility and Range of Motion
The repeated leg extension involved in backward walking can improve your flexibility, particularly in your hamstrings and ankles. This can help with overall range of motion and reduce stiffness.
Burns more Calories
Studies suggest that walking backwards may burn slightly more calories than walking forward, although the difference is small.
Diabetics have ways to fast safely: ACEDB
Association of Clinical Endocrinologists and Diabetologists of Bangladesh (ACEDB) on Friday diabetes patient can fast easily by following some rules as modern medical methods have made fasting easy and safe.
ACEDB informed this info in an event organized at National Press Club. The event was organized on the occasion of Dia-Ramadan Awareness Month program announced by ACEDB for the month of Rajab.
In addition to the month-long program of the organization, some programs were highlighted to safely observe the fasting of diabetic patients.
According to ACEDB, fasting is one of the five pillars of Islam. So, fasting is a must for every adult Muslim. Research has shown that about 80 percent of diabetic patients in Bangladesh maintain fast.
According to a statistic, around 50 million diabetics patients around the world fast. But among diabetic patients who maintain fast without doctor's advice, they face some complications. In particular, suffer from low blood sugar (hypoglycemia), high blood sugar (hyperglycemia), diabetic ketoacidosis, and dehydration.
Former Secretary of Ministry of Health and Family Welfare Dr. Anwar Hossain Howlader said in the speech as chief guest, several recent studies shown, those who fast with the preparation of Ramadan have less complications including hypoglycemia than before Ramadan. Various studies have proven that fasting is beneficial to health.
"Diabetic patients are advised to consult their doctor at least 2-3 months before Ramadan to prepare," he said.
ACEDB President Professor Farid Uddinsaid, Muslims want to fast this one month for self-purification. Diabetics patients are no exception. Since fasting requires long periods of fasting and diabetics patients who take insulin or take oral medication, they need to take special precautions during Ramadan.
He also said it is necessary to plan and take advance preparation. You can combine diet, exercise and medicine. You can practice Nafal fasting before Ramadan.
General Secretary of ACEDB Prof. Dr. Indrajit Prasad said, some issues can be solved own by thinking a little consciously. For example, talk to the doctor and bring 3 times the medicine in one or two times. Can take day medicine at night before Ramadan.Experts of the organization said that diabetic patients can fast.
"Diabetes is not a barrier for those who can afford it. Prior preparation is required. They advised, diabetic patients should consult their doctor at least 2-3 months before Ramadan and make preparations," he also advised.
According to the ACEDB, several recent studies have shown that those who maintain fast with the preparation of Ramadan have a much lower incidence of hypoglycemia and other complications than before Ramadan. Various studies have proven that fasting is beneficial for health.
In the event, they informed that the Endocrine Department of Bangabandhu Sheikh Mujib Medical University has been taking various programs to make people aware at all levels about the safe fasting of diabetic patients. Before Ramadan, the endocrinologists of this hospital have been conducting various programs across the country.
Association of Clinical Endocrinologists and Diabetologists of Bangladesh (ACEDB), the leading organization of endocrinologists in Bangladesh, has declared the month of Rajab as 'Diabetes and Ramadan Awareness Month' in October 2023 to highlight the important issue more seriously to the countrymen.
In continuation of that, on the first Friday of the month of Rajab, on January 27, 2023, its auspicious opening was announced at the Dhaka Club, which is the first time in the world.
Programs for the month of Rajab include – training of doctors, training of diabetic patients, discussions with mosque khatibs and raising public awareness through various media.
ACI Pharmaceuticals Limited is cooperating in this regard.